Key Takeaways
-
- Up to 30 percent of people who have psoriasis will later develop psoriatic arthritis (PsA).
- Figuring out which people with psoriasis may be more likely to go on to develop psoriatic arthritis is an important area of research.
- New research suggests that people with moderate to severe psoriasis are more likely to develop PsA.
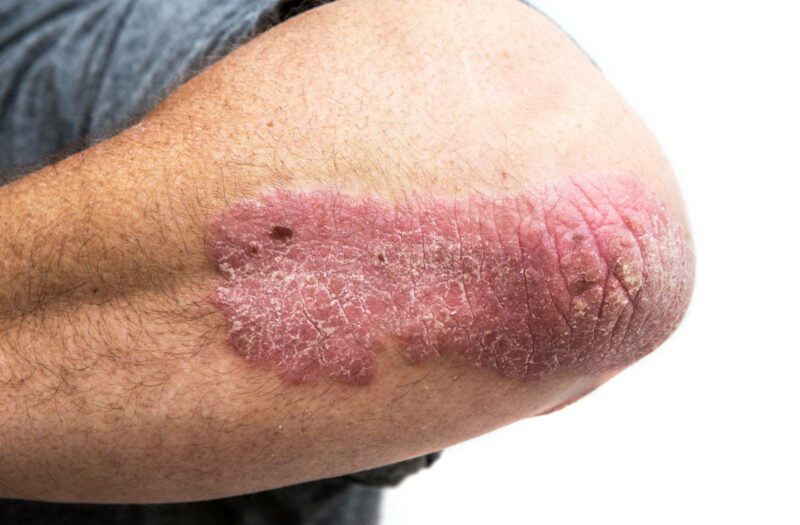
Psoriasis and psoriatic arthritis (PsA) are two conditions that are closely related. Both are caused by unchecked inflammation; psoriasis is characterized by skin cells that build up rapidly, causing thick, scaly patches. In psoriatic arthritis, people also develop inflammation and pain in the joints and the locations where tendons or ligaments attach to your bone, called entheses.
Psoriasis often leads to the development of psoriatic arthritis; in fact, data indicates that up to 30 percent of people who have psoriasis will later develop psoriatic arthritis. (In other cases, people develop psoriasis and psoriatic arthritis at the same time, and in some instances people develop arthritis first, followed by psoriasis symptoms later.)
Figuring out which people with psoriasis may be more likely to go on to develop psoriatic arthritis is an important area of research, because this may ultimately lead to ways to prevent the onset of PsA in those at high risk.
A growing body of evidence suggests that psoriasis severity might be one such risk factor worth paying attention to, according to a recent study in the Journal of the American Academy of Dermatology.
Researchers, led by Joseph F. Merola, MD, a Harvard Medical School professor and doctor who is board-certified in both dermatology and rheumatology, looked at the incidence, prevalence, and predictors of psoriatic among people diagnosed with psoriasis, stratifying them by the severity of their condition.
The researchers evaluated patient data from the Optum electronic health records database. They found that out of every 100 years of patient data reviewed, an average of 2.9 psoriatic arthritis occurrences took place.
But when the researchers reviewed those occurrences depending on the severity of a patient’s psoriasis, the average rate of PsA occurrences changed.
- For every 100 years of data for patients with mild psoriasis, PsA occurrences averaged 2.1.
- For every 100 years of data for patients with moderate psoriasis, PsA occurrences increased to 9.9.
- For every 100 years of data for patients with severe psoriasis, there were 17.6 occurrences of PsA.
The data indicates a significant increase in PsA development for patients with moderate to severe psoriasis, and it provides important information about the link between these conditions. While more research is needed, this study indicates that the risk of developing psoriatic arthritis increases with worse psoriasis disease severity.
The authors noted that “patients with psoriasis should be routinely screened by dermatologists for subclinical signs and symptoms of psoriatic arthritis, especially those who have more-severe disease and other risk factors.”
As we learn more about how psoriasis severity affects the risk of developing PsA, doctors and patients should be more vigilant about monitoring for symptoms of psoriatic arthritis. This could lead to a faster diagnosis and more prompt treatment to help control PsA symptoms and prevent long-term complications.
It is very important for psoriasis patients to pay attention to signs of joint pain, stiffness, and swelling and let your doctor know if you’re experiencing them.
Treatment for psoriasis typically falls into three broad categories: topical creams and ointments that treat inflammation locally in the skin, phototherapy (UV light treatments) and systemic medications (including oral pills and injectable biologics) that address underlying inflammation by affecting immune system function. You and your doctor should work together to create a treatment plan that addresses your symptoms.
If your psoriasis is not responding well to topical treatment, covers a large portion of your body’s surface, is in places that are hard to treat topically (such as the scalp), or is having a negative impact on your quality of life (affecting your mental health, work, or relationships), that’s a sign you may be a good candidate for more aggressive treatment to get your psoriasis under better control — and possibly reduce the risk of progressing to PsA.
Track Your Symptoms with ArthritisPower
Join CreakyJoints’ patient-centered research registry and track symptoms like fatigue and pain. Sign up.
Merola JF, et al. Incidence and Prevalence of Psoriatic Arthritis in Patients With Psoriasis Stratified by Psoriasis Disease Severity: Retrospective Analysis of a US Electronic Health Records Database. Journal of the American Academy of Dermatology. September 18, 2021. doi: https://doi.org/10.1016/j.jaad.2021.09.019.