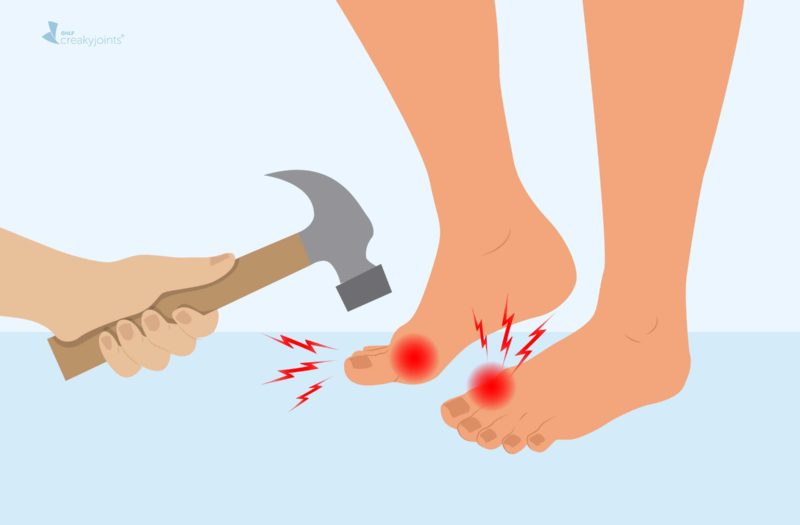
For CreakyJoints member Louise B., her gout flares hit at the base joint of her right big toe, which is a common joint for gout.
It starts with a tingling sensation and some swelling and rapidly becomes extremely painful, very swollen, and red. “This pain is off the charts, completely intolerable,” she shared in response to a recent Facebook post asking people what gout pain feels like.
When Ross W. had his first gout attack while on a bachelor party ski trip a few years ago, he thought he broke his toe. He spent the weekend hobbling — unable to hit the slopes — and rushed to see a podiatrist upon his return. As a teenager, Ken L., who is now in his sixties, started experiencing foot pain that he chalked up to playing street hockey. But once he started having trouble walking and even putting his foot in a shoe, he knew it had to be more than just an injury.
For other patients, gout attacks tend to strike in places beyond the toes and feet. Soledad B. shared that her gout flares in her elbows, for example.
What Is Gout?
Gout is the most common type of inflammatory arthritis, affecting more than 9 million adults in the U.S., according to recent data. Gout is a condition that develops when the body has high levels of uric acid, a normal waste product. Uric acid is normally excreted through the body via the kidneys, but in some people, levels can remain high and uric acid can start to accumulate and crystallize in various joints. This is what triggers a telltale gout attack.
While gout can flare in many different joints, pain and inflammation are the hallmark symptoms.
“A gout attack is usually not subtle,” says John D. FitzGerald, MD, PhD, a rheumatologist and internationally recognized expert in gout diagnosis and treatment at the David Geffen School of Medicine at UCLA Medical Center in Los Angeles.
Unlike other types of arthritis that may cause more of a dull, aching chronic pain and stiffness, a gout flare tends to come on quickly. Dr. FitzGerald describes a gout flare as sudden onset and very painful in a joint, often at the base of the first big toe, but advises that gout can attack almost any other joint, which can make it difficult to recognize.
Joints Affected by Gout
Depending on which joint(s) flare with gout, the pain and effects of the inflammation can cause different issues. Here is a list of joints vulnerable to gout flare and how the pain might affect you, according to Hospital for Special Surgery.
Common joints for gout attack:
- Big toe: Sudden pain that is tender to the touch, visibly red, and difficult to put weight on
- Mid-foot: Tingling, followed by increased onset of pain that can be difficult to put weight on
- Ankle: Burning and tingling pain and swelling that can prevent walking
- Knee: Burning pain and swelling that can prevent leg movement
- Elbow: Radiating pain that can restrict arm movement
Less common joints for gout attack that are often impacted as gout progresses and worsens:
- Fingers: Burning pain, redness, and decreased range of motion
- Wrist: Burning pain, redness, and restricted movement
- Shoulder: Gout very rarely attacks the shoulder
Hard deposits of uric acid, called tophi, can develop with gout. These deposits grow under the skin around cartilage, such as at the top of the ear, and around joints and can be diagnosed as chronic tophaceous gout, according to Johns Hopkins Arthritis Center.
If gout flares persist without treatment, there can be permanent damage to the joint, leading to impaired movement.
What Causes Gout Pain
Picture a collection of glass shards pressing outward like needles. This is what it can feel like during a gout flare, when a buildup of uric acid in the blood (called hyperuricemia) forms microscopic crystals that grow in and around a joint. As the build-up increases, the immune system responds to these crystals, causing inflammation that leads to visible swelling, redness, and debilitating pain.
In some cases, a gout flare can even lead to a fever and look like an infected joint, Dr. FitzGerald notes. “The treating doctor may need to look for possible source of infection, often by removing fluid from the joint to send to the lab to look for crystals or bacteria.”
Uric acid is a byproduct of the body breaking down proteins called purines from your own cells and from certain foods such as red meat and shellfish. Alcohol and drinks sweetened with high fructose corn syrup are also high in purines. Normally, uric acid dissolves in your blood and is filtered out through your kidneys, but when your body produces too much uric acid or your kidneys fail to filter it, either due to familial (genetic) causes or kidney disease, then the uric acid builds up and creates the needle-like urate crystals that cause gout and can also form kidney stones, according to the Mayo Clinic.
Certain factors make some people more likely to develop gout, according to the U.S. Centers for Disease Control and Prevention. Gout risk factors include:
- Male sex
- Obesity
- Health conditions such as high blood pressure, diabetes, or poor kidney function
- Taking certain medications, such as diuretics (water pills)
- Eating a lot of high-purine foods, including alcohol, sugar, red meat, and seafood and shellfish
How Long Gout Pain Lasts
“Characteristically, gout pain comes on rapidly and the joint becomes red and swollen, with the swelling reaching a peak within the first 24 hours of the attack,” Dr. FitzGerald explains.
At first, gout usually affects just one joint, but can affect more than one joint, sometimes adjacent joints. Flares typically resolve on their own over the next seven to 14 days. Treating a gout flare with medications can help it resolve faster. Medications for gout flares typically include:
- Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen
- Colchicine
- Glucocorticoids (steroids)
A gout attack may occur only one or two times a year or even only a few times ever. However, gout can become chronic, leading to frequent attacks and flares that occur at least a few times a year or never completely resolve. Chronic gout can damage and deform joints and can sometimes be mistaken for other inflammatory diseases like rheumatoid arthritis.
Signs Your Pain Is Likely Gout and Not Something Else
If you develop sharp sudden pain in a single joint or a couple of joints, if the pain is so debilitating that it is hard to walk or wear shoes, and if you have risk factors for gout (especially a family history), there’s good reason to suspect gout as the culprit. However, it’s important to see a doctor for a thorough exam and proper diagnosis.
Dr. FitzGerald cautions that issues unrelated to gout can cause an angry, inflamed joint. Gout may be confused with several other conditions that can cause similar symptoms, including:
- Pseudogout
- An infected joint (septic arthritis)
- Bacterial skin infection (cellulitis)
- Stress fracture
- Rheumatoid arthritis
- Psoriatic arthritis
Pseudogout (technical term calcium pyrophosphate dihydrate deposition disease) is caused by a different kind of crystal, calcium pyrophosphate. A flare of pseudogout can resemble gout, but it more often affects your wrist and knee, and is unlikely to involve the big toe. Like gout, pseudogout is also considered a form of inflammatory arthritis. It’s more likely to affect people over the age of 40 and those who have a thyroid condition, kidney failure, or disorder that affects calcium, phosphate, or iron metabolism, according to the Cleveland Clinic.
It’s also possible to have gout without the classic presentation of red, hot, sharp, burning, sudden pain in the big toe, foot, ankle, or knee. Some patients may have joint pain that is less acute.
People can also have high levels of uric acid but not develop symptoms of gout.
What to Do If You Think You Have Pain Due to Gout
The good news is that there are effective medications to treat gout, Dr. FitzGerald says. In some mild cases, gout can be self-managed with lifestyle changes, such as weight loss if needed and eating fewer high-purine foods (alcohol, sugar-sweetened beverages, red meat, and seafood).
However, many people with gout should be on a preventive medication to lower uric acid levels and stop flares from occurring. According to the 2020 gout treatment guidelines from the American College of Rheumatology, uric acid-lowering medication is recommended for people who:
- Have two or more gout flares a year
- Have gout tophi
- Have evidence on X-rays of joint damage due to gout
The guidelines, of which Dr. FitzGerald is a coauthor, recommend a “treat-to-target” strategy, which means treating gout with medication until a target uric acid level is reached.
Unfortunately, gaps in quality care for gout continue to persist and many patients do not take uric acid-lowering medication, which can leave people suffering the intense and persistent pain of gout without relief. This is why it is important to seek medical care if you experience pain that you think could be gout, Dr. FitzGerald stresses.
Gout can be diagnosed several ways, including:
- Removing fluid from the joint to identify urate crystals.
- Using ultrasound to identify several common characteristics of gout, such as collections of crystals in or around joints.
- Using dual-energy CT (computed tomography) to detect urate crystal deposits in cases that are more advanced.
Treating and Preventing Gout Pain
Gout pain is generally treated in two ways:
- Medications to relieve gout attacks in the short-term
- Preventive medications taken regularly to lower uric acid and stop gout attacks from occurring
While inflammation-fighting drugs (NSAIDs, colchicine, and glucocorticoids) are used to relieve pain during gout flares, different medicines are used to lower uric acid levels to prevent future attacks. These include:
- Allopurinol (the most commonly used medication to lower uric acid levels)
- Febuxostat
- Probenecid
Another medication called pegloticase (Krystexxa) may be recommended for people with chronic gout who have not responded to other uric acid-lowering medication.
While many people with gout can be treated by their primary care physician, if gout is not responding to medication or is progressing with worsening or frequent flares or developing tophi gout deposits, then your primary care physician may refer you to see a rheumatologist who specializes in treating diseases that affect joints, muscles, bones and the immune system.
Taking medication to reduce uric acid levels and reduce the risk of gout progression is important, Dr. FitzGerald stresses. “If you have risk factors for bad gout, such as kidney disease, or are experiencing frequent attacks, early treatment is better.”
Not Sure What’s Causing Your Pain?
Check out PainSpot, our pain locator tool. Answer a few simple questions about what hurts and discover possible conditions that could be causing it. Start your PainSpot quiz.
Calcium Pyrophosphate Dihydrate Deposition Disease (CPPD, or Pseudogout). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/4756-calcium-pyrophosphate-dihydrate-deposition-disease-cppd-or-pseudogout.
Chen-Xu M, et al. Contemporary prevalence of gout and hyperuricemia in the United States and decadal trends: the National Health and Nutrition Examination Survey, 2007–2016. Arthritis & Rheumatology. January 2019. doi: https://doi.org/10.1002/art.40807.
FitzGerald, et al. 2020 American College of Rheumatology Guideline for the Management of Gout. Arthritis Care & Research. June 2020. Doi: https://doi.org/10.1002/art.41247.
Gout. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/gout/symptoms-causes/syc-20372897.
Gout: Risk Factors, Diagnosis and Treatment. Hospital f0r Special Surgery. https://www.hss.edu/conditions_gout-risk-factors-diagnosis-treatment.asp.
Gout. U.S. Centers for Disease Control and Prevention. https://www.cdc.gov/arthritis/basics/gout.html.
Interview with John D. FitzGerald, MD, PhD, a rheumatologist and internationally recognized expert in gout diagnosis and treatment at the David Geffen School of Medicine at UCLA Medical Center in Los Angeles
Neogi T, et al. 2015 Gout Classification Criteria: An American College of Rheumatology/European League Against Rheumatism Collaborative Initiative. Annals of the Rheumatic Diseases. October 2015. doi: http://dx.doi.org/10.1136/annrheumdis-2015-208237.
Symptoms and Diagnosis of Gout. Johns Hopkins Arthritis Center. https://www.hopkinsarthritis.org/arthritis-info/gout/clinical-presentation-of-gout.