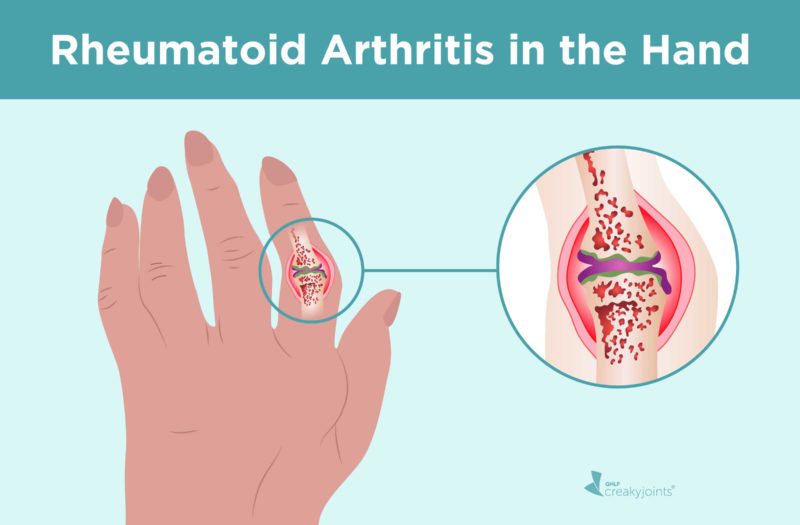
Your hand is one of the most complex structures in the human body. It’s designed to give powerful grip, lift heavy objects, and manipulate small ones (like threading a fine string through a tiny needle eye). Made up of the wrist, palm, and fingers, each hand contains 27 small joints, the same number of bones, and a whole lot of muscles, tendons, and ligaments. All of this complexity also makes the hand a prime target for rheumatoid arthritis (RA).
Rheumatoid arthritis is a chronic, inflammatory disease in which your immune system mistakenly attacks the lining of the membrane that surrounds your joints. Though RA can affect joints and organs all over the body, it often strikes in smaller joints first — particularly those in your hand and wrist, as well as ones in your feet.
Research suggests an estimated 90 percent of people will RA experience pain, stiffness, or swelling in joints in their hand, and often results in problems performing daily activities.
Read more here about common rheumatoid arthritis symptoms.
How Rheumatoid Arthritis Affects Your Hands
Many joints are covered with a lining called the synovium, which lubricates the joint so it moves more easily. When you have rheumatoid arthritis, the synovium becomes inflamed, thickens, and produces an excess of joint fluid. This is known as synovitis. That extra fluid — along with the inflammatory chemicals released by the immune system — causes swelling, damages cartilage, and softens the bone within the joint. The swollen tissue may stretch the surrounding ligaments, resulting in deformity and instability, according to the American Society for Surgery of the Hand. The inflammation may also weaken and damage tendons. Ligaments are connective tissues that join two bones; tendons are connective issues that join muscle to bone.
When RA strikes the hand, it is most common in the wrist and finger knuckles — more specifically the MCP (metacarpophalangeal) joint, or the large knuckle where the fingers and thumb meet the hand, and the PIP (proximal interphalangeal) joint, or middle knuckle, explains Jemima Albayda, MD, Assistant Professor of Medicine in the Division of Rheumatology at Johns Hopkins Medicine in Baltimore.
The first knuckle at the top of the finger closest to the nails — the DIP, or distal interphalangeal joint — is generally spared in RA. (It is more often involved in other types of arthritis such as osteoarthritis or psoriatic arthritis.) In the wrist, RA often affects the joint between the two bones of the forearm, the radius and ulna.
RA tends to involve the small joints of the hands and feet early on in the disease process, adds Dr. Albayda, who also serves as the Director of the Musculoskeletal Ultrasound and Injection Clinic at Johns Hopkins.
In fact, one study in the Journal of Rehabilitation Medicine that included 200 patients with rheumatoid arthritis found that 94 percent had at least one hand or wrist symptom, and 67 percent had at least one related impairment, mostly from the earliest stages onward.
What Does Rheumatoid Arthritis in the Hands Feel Like?
When your hands are affected by rheumatoid arthritis, you may experience swelling around the affected joint, which leads to pain or tenderness. The joint may feel warm to the touch. Swelling tends to be symmetrical, which means it occurs in the same joints on both right and left hands.
Stiffness with immobility is characteristic of rheumatoid arthritis in the hands as well, says Lindsay S. Lally, MD, a rheumatologist at Hospital for Special Surgery in New York City. Symptoms like stiffness and pain are usually worse in the morning, and can last at least 30 minutes or more.
Together these hand symptoms can impair function and the ability to go about your daily routine and tasks.
“This can manifest in difficulty using the fingers, decreased hand dexterity, inability to bend or straighten affected joints, and decreased strength,” says Dr. Albayda. “Sometimes RA can cause loosening of ligaments and tendons in the hands, resulting in permanent deformities of the hand,” adds Dr. Lally. Evidence suggests that hand deformities commonly occur in the first year of rheumatoid arthritis if it goes untreated.
Some specific hand problems and deformities that can be caused or made worse by rheumatoid arthritis include:
Carpal tunnel syndrome
The carpal tunnel is a narrow passageway surrounded by ligament and bone. It is located at the base of your hand and houses tendons and the median nerve, which runs from your forearm into the palm of your hand. Any pressure on this major nerve in your wrist causes tingling, numbness, or weakness in your hand and arm.
Because RA can cause swelling and inflammation in the wrist, this can compress the median nerve and lead to carpal tunnel syndrome, explains Dr. Albayda.
Trigger finger
The medical term for trigger finger is stenosing tenosynovitis. It occurs when the protective sheath, or lining, that surrounds a tendon becomes irritated and inflamed (tenosynovitis). Its more common moniker stems what happens next: inflammation interferes with the normal gliding motion of the tendon through the sheath, and the affected finger gets stuck in a bent position. Your finger may bend or straighten with a snap — like a trigger being pulled and released, according to the Mayo Clinic. In severe cases, your finger may become locked in a bent position. Rheumatoid arthritis is a risk factor for trigger finger.
Ulnar drift
Also known as ulnar deviation, this hand condition is a unique sign of rheumatoid arthritis, according to the American Society for Surgery of the Hand. It occurs when the large knuckle bones become so swollen and damaged that your fingers begin to bend abnormally and drift sideways, away from your thumb and toward the ulna bone in the forearm (located on the pinky side).
Swan’s neck deformity
This occurs when the middle joint on the finger bends back more than normal (or hyperextends), and the top joint is flexes, or bends down, resulting in a shape that resembles a swan’s neck.
Boutonniere deformity
Sometimes called a buttonhole deformity, the middle finger joint is bent in (toward the palm) and the top finger joint is bent out (away from the palm).
Hitchhiker’s thumb
Your thumb’s large knuckle abnormally flexes while the top knuckle hyperextends, resembling a Z-shape.
Rheumatoid nodules
Some people with RA will develop hard lumps under the skin called nodules, often around pressure points. In the hands, nodules may appear on finger joints and wrists.
Signs Your Hand Pain Is Not Due to Rheumatoid Arthritis
Pain and stiffness in the hand are hallmark signs of rheumatoid arthritis, but these symptoms can stem from many other different conditions.
“Sometimes, it can be very difficult to make the distinction of whether current symptoms in the hand are from ongoing inflammation, from damage or another condition like OA, or a whole other entity,” says Dr. Albayda.
Some clues that your hand pain may not stem from rheumatoid arthritis include:
Hand pain is worse with activity
This type of hand pain tends to occur in osteoarthritis (OA), a degenerative disorder where the cartilage that cushions the end of a joint breaks down over time. Joint symptoms of OA are more likely to be exacerbated by repetitive or overuse and effort, explains Dr. Lally — for example, gardening or crafting.
In RA, on the other hand, pain and stiffness tend to come with lack of use and after periods of inactivity, such as when you wake up in the morning after being still all night.
Another way to distinguish the two: swelling in your hand and wrist is hard and bony in OA; boggy and squishy in RA, says Dr. Albayda.
Fingers swell like sausages
Psoriatic arthritis (PsA) is another form of inflammatory arthritis that can cause painful, swollen joints that are warm to the touch. Psoriatic arthritis, however, is more likely to also cause sausage-like swelling in the fingers and toes (called dactylitis).
Also, pain and stiffness in the first knuckle of the finger tends to occur in psoriatic arthritis, as well as osteoarthritis, but rarely seen in RA, says Dr. Lally.
Read more here about psoriatic arthritis symptoms.
You have a butterfly-shaped rash on your face
This rash gets its name because it spans the cheeks and bridge of the nose, creating a shape similar to a butterfly spreading its wings. It’s a telltale sign of lupus, an autoimmune disease that shares many symptoms with RA — including pain, stiffness, and swelling in the fingers and wrists. Learn more here about symptoms that are distinct to lupus.
Other conditions that can cause hand pain include:
Carpal tunnel syndrome
Rheumatoid arthritis can raise your risk of this condition, but many other factors can contribute as well, including anatomy of your wrist, nerve-damaging diseases and possibly repetitive hand motions. It’s tricky because you could have carpal tunnel syndrome that is related to RA or not at all related to RA.
Ganglion cyst
These are soft, round, noncancerous lumps that most commonly develop along the tendons or joints of your wrist or hand. If it presses on a nearby nerve, it can cause pain, numbness or weakness.
Tendon problems
Tendonitis (inflammation of the tendon) and tenosynovitis (inflammation of the protective lining of the tendon) can cause symptoms in the wrist and fingers.
Traumatic injuries
Injuring your hand in an accident or while exercising or playing sports can cause acute pain that can linger and become chronic.
How RA Hand Pain Is Diagnosed
There’s no one test to diagnose RA — and in its early stages, signs and symptoms can mimic those of many other diseases.
But early diagnosis of rheumatoid arthritis is important for the best outcome. “We are learning that we need to control inflammation much more aggressively upfront as joint damage can ensue early on,” says Dr. Albayda. “Hence, there has been a shift in treatment paradigms to catching patients early and instituting treat-to-target control.”
To help determine whether you have RA in your hand or wrist, a health care provider will examine your hands and fingers for such symptoms as:
- Swelling
- Redness and warmth
- Reduced range of motion
- Pain
- Joint instability
They will also ask questions about other symptoms that tend to go along with RA, such as fatigue, flu-like symptoms, fever, and disrupted sleep.
A health care provider may order imaging tests to check for certain characteristics of RA, such as narrowing of the joint space or erosions of the bone. They will run blood tests to look for antibodies (proteins found in the bloodstream) that may be found in people with RA as well as elevated levels of markers of inflammation in the blood.
Here is more information about tests used for diagnosing rheumatoid arthritis and criteria used for diagnosing rheumatoid arthritis.
How RA Hand Pain Is Treated
There is no cure for rheumatoid arthritis, but there is a lot you can do to relieve symptoms, prevent damage, and maintain function in your hands. To help keep your hands healthy:
1. Stick to your prescribed rheumatoid arthritis treatment plan
Medication that helps reduce out-of-control inflammation in the body is a cornerstone of rheumatoid arthritis treatment. Depending on the severity of your symptoms and how long you’ve had rheumatoid arthritis, your rheumatologist may prescribe a combination of medications. “One of the major goals of treatment of RA is to prevent this structural damage that can result in loss of dexterity and strength in the hands,” says Dr. Lally.
Commonly prescribed medications include:
Nonsteroidal anti-inflammatory drugs (NSAIDs)
These medications, such as ibuprofen or naproxen or prescription versions, are used for mild joint pain and reduce inflammation but don’t prevent disease progression.
Glucocorticoids
These medications, such as prednisone, help reduce inflammation quickly and tend to be prescribed during flares. They used sparingly and carefully in people with RA because they can have a wide range of side effects.
Disease-modifying anti-rheumatic drugs (DMARDs)
These medications address the underlying systemic inflammation in rheumatoid arthritis. They are critical for slowing and stopping the course of inflammatory disease. They fall into three general categories.
- Conventional disease-modifying antirheumatic drugs (DMARDs), which are often taken orally and include medication such as methotrexate, hydroxychloroquine, and sulfasalazine.
- Targeted disease-modifying antirheumatic drugs (DMARDs), which are oral pills that are more targeted than conventional DMARDs [ex: a JAK inhibitor like tofacitinib (Xeljanz), baricitinib (Olumiant), or upadacitinib (Rinvoq)]
- Biologic disease-modifying antirheumatic drugs (DMARDs),which are administered as injections or infusions and are more targeted than conventional DMARDs [ex: a TNF inhibitor like adalimumab (Humira) or etanercept (Enbrel), an IL-6 inhibitor like tocilizumab (Actemra) or sarilumab (Kevzara), an IL-1 inhibitor like anakinra (Kineret), a T cell inhibitor like abatacept (Orencia), or a B cell inhibitor like rituximab (Rituxan)]
“The treatments that we have for RA — both the conventional DMARDs such as methotrexate and the biologics and JAK inhibitors — can help improve joint pain, swelling, and stiffness while preventing the development of long-term damage,” adds Dr. Lally.
2. See a physical or occupational therapist
Your doctor may refer you to a physical or occupational therapist to help maintain hand function and dexterity and strengthen joints, say experts. Depending on your needs, a therapist may give you exercises to improve range of motion and function in your hand and wrist, recommend the use of splints or braces to help support joints and ease stress, and suggest new ways to do everyday tasks that may help relieve pain and protect your joints.
Here are some arthritis-friendly hand exercises you can do regularly.
3. Apply heat or cold
A warm compress can help ease pain and stiffness, cold can help ease inflammatory symptoms, such as swelling. Try both to see which works best for you, or alternate between the two. Here are simple ways to do hot therapy and cold therapy at home.
4. Modify your movements
If certain activities aggravate your arthritis, find ways to cut down or eliminate them to help minimize your symptoms. For example, if you spend long hours typing on a computer, you may need to take regular breaks or work in shorter spurts. Or consider voice recognition software to give your hands and wrist a break. Read more here about how to type and text with less pain.
5. Use assistive devices
From easy-grip kitchen and gardening tools to button hooks and dressing sticks, there are tons of productsspecifically designed to reduce pain, lessen strain, and help protect your finger and wrist joints. Don’t want to invest in another gadget? Here are expert-recommended household items that might help you manage your arthritis too — without spending a dime.
6. Consider a steroid injection
Cortisone injections into the affected joint can help reduce inflammation. The catch: It’s a temporary fix, and it won’t stop the progression of the disease.
7. Talk to your doctor about surgery options
“If pain is unrelenting or there is loss if function in the hands, your rheumatologist may refer you for a surgical evaluation, particularly when there’s an anatomic defect that can be corrected,” says Dr. Albayda.
Surgery may involve removal of inflamed joint linings, tendon repair, joint fusions, or joint replacements. Depending on the joint involved, the degree of damage, and other factors, you hand surgeon will determine the most appropriate treatment to help correct deformities, relieve pain, or improve function.
Track Your Rheumatoid Arthritis Symptoms with ArthritisPower
Join CreakyJoints’ patient-centered research registry and track symptoms like fatigue and pain. Learn more and sign up here.
Watch: Getting Started on Rheumatoid Arthritis Medications
This video is part of an educational project from researchers at Yale University, Berkshire Medical Center, Carnegie Mellon University, Hospital for Special Surgery, CreakyJoints and the Global Healthy Living Foundation, and ArthritisPower. It was made possible with support from the Rheumatology Research Foundation. Watch more videos from this series here.
If you enjoyed reading this article, you’ll love what our video has to offer.
Arthritis of the Hand. OrthoInfo. American Academy of Orthopaedic Surgeons. December 2013. https://orthoinfo.aaos.org/en/diseases–conditions/arthritis-of-the-hand.
Arthritis of the Wrist. OrthoInfo. American Academy of Orthopaedic Surgeons. April 2016. https://orthoinfo.aaos.org/en/diseases–conditions/arthritis-of-the-hand.
Boutonniere Deformity. Hand Care. 2017. American Society for Surgery of the Hand.https://www.assh.org/handcare/condition/boutonniere-deformity.
Boutonnière Deformity. Merck Manual Consumer Version. https://www.merckmanuals.com/home/bone,-joint,-and-muscle-disorders/hand-disorders/boutonni%C3%A8re-deformity.
Carpal Tunnel Syndrome. Hand Care. 2015. American Society for Surgery of the Hand. https://www.assh.org/handcare/condition/carpal-tunnel-syndrome.
Carpal Tunnel Syndrome Fact Sheet. National Institute of Neurological Disorders and Stroke. U.S. National Institutes of Health. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Carpal-Tunnel-Syndrome-Fact-sheet.
Ellegard K, et al. Hand exercise for women with rheumatoid arthritis and decreased hand function: an exploratory randomized controlled trial. Arthritis Research & Therapy. June 2019. doi: https://doi.org/10.1186/s13075-019-1924-9.
Explain the pain – Is it osteoarthritis or rheumatoid arthritis? Harvard Health Publishing. https://www.health.harvard.edu/pain/explain-the-pain–is-it-osteoarthritis-or-rheumatoid-arthritis.
Fleming A, et al. Early rheumatoid disease. II. Patterns of joint involvement. Annals of the Rheumatic Diseases. August 1976. doi: http://dx.doi.org/10.1136/ard.35.4.361.
Ganglion Cyst. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/ganglion-cyst/symptoms-causes/syc-20351156.
Hand Anatomy. Orthopedics Northwest. https://www.orthonw.com/hand-anatomy-orthopedics-northwest-tigard-oregon.html.
Hand Pain and Problems. Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/conditions-and-diseases/hand-pain-and-problems.
Hitchhiker thumb deformity. Radiopaedia. https://radiopaedia.org/articles/hitchhiker-thumb-deformity.
Horsten NC, et al. Prevalence of hand symptoms, impairments and activity limitations in rheumatoid arthritis in relation to disease duration. Journal of Rehabilitation Medicine. November 2010. doi: https://doi.org/10.2340/16501977-0619.
How Do Hands Work? InformedHealth.org. Institute for Quality and Efficiency in Health Care. July 26, 2018. https://www.ncbi.nlm.nih.gov/books/NBK279362.
Interview with Jemima Albayda, MD, Assistant Professor of Medicine in the Division of Rheumatology at Johns Hopkins Medicine in Baltimore
Interview with Lindsay S. Lally, MD, a rheumatologist at Hospital for Special Surgery in New York City
Johnsson PM. Hand deformities are important signs of disease severity in patients with early rheumatoid arthritis. Rheumatology. November 2009. doi: https://doi.org/10.1093/rheumatology/kep253.
Lupus. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/lupus/symptoms-causes/syc-20365789.
Misra DP, et al. Rheumatoid Hand. Journal of Clinical Rheumatology. June 2015. doi: https://doi.org/10.1097/RHU.0000000000000253.
Osteoarthritis. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925.
Psoriatic Arthritis. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/psoriatic-arthritis/symptoms-causes/syc-20354076.
Rheumatoid Arthritis. American College of Rheumatology. https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Rheumatoid-Arthritis.
Rheumatoid Arthritis. Hand Care. 2017. American Society for Surgery of the Hand. https://www.assh.org/handcare/condition/rheumatoid-arthritis.
Rheumatoid Arthritis. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/rheumatoid-arthritis/symptoms-causes/syc-20353648.
Rheumatoid arthritis & Computing. National Rheumatoid Arthritis Society. https://www.nras.org.uk/rheumatoid-arthritis-computing.
Rheumatoid Arthritis Signs & Symptoms. Johns Hopkins Arthritis Center. https://www.hopkinsarthritis.org/arthritis-info/rheumatoid-arthritis/ra-symptoms.
Rheumatoid nodules. National Rheumatoid Arthritis Society. https://nras.org.uk/resource/rheumatoid-nodules.
Swan-Neck Deformity. Merck Manual Consumer Version. https://www.merckmanuals.com/home/bone,-joint,-and-muscle-disorders/hand-disorders/swan-neck-deformity.
Swan Neck Deformity. Hand Care. 2017. American Society for Surgery of the Hand. https://www.assh.org/handcare/condition/swan-neck-deformity.
Trigger Finger. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/trigger-finger/symptoms-causes/syc-20365100.