
If you live with arthritis, chances are you feel the painful effects in your feet. “Feet are tremendously affected by arthritis,” says Vinicius Domingues, MD, a rheumatologist in Daytona Beach, Florida, and medical advisor for CreakyJoints.
Indeed, osteoarthritis (OA), the most common type of arthritis, affects the feet of one in six people over the age of 50. With rheumatoid arthritis (RA), the most common type of inflammatory autoimmune arthritis, more than 90 percent of patients develop symptoms in the foot and ankle over the course of the disease. In about 20 percent of RA cases, foot and ankle symptoms are even among the first signs of the disease.
It’s not surprising that you can feel arthritis in your feet: The disease predominantly affects your joints, and your foot contains more than 30 joints.
How Different Kinds of Arthritis Hurt Your Feet
Various types of arthritis present differently in the feet.
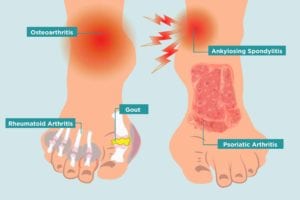
- Osteoarthritis most commonly affects the first metatarsophalangeal joint (MTP) that connects your big toe to your foot, although it’s also often found in the midfoot and ankle.
- Rheumatoid arthritis usually appears in both feet and affects the same joints in each foot. This is in contrast to OA, which typically affects one specific joint.
- Gout frequently affects only the feet, often the big toe. Read more about treating a gout flare.
- Psoriatic arthritis (PsA) can also take a toll on toes, causing sausage-like swelling called dactylitis. PsA is often also accompanied by inflammation of the entheses, the places where tendons and ligaments attach to bones. In the feet this usually presents as plantar fasciitis, an inflammation of the band of tissue that connects the heel bone to the toes, as well as the bony projections known as bone spurs, which can cause pain if they press or rub on other bones or soft tissues.
- Ankylosing spondylitis also causes enthesitis, such as plantar fasciitis and pain at the Achilles tendon.
How to Heal Arthritis Foot Pain
Now that we’ve established why your feet are hurting, consider these strategies for easing the pain, stiffness, and swelling that arthritis patients often know all too well.
1. Use pain meds
Available in both over-the-counter and prescription versions, nonsteroidal anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen, and naproxen are a top-line treatment for reducing the pain, swelling, and redness associated with arthritis, including when arthritis strikes in the feet. NSAIDS help block the production of prostaglandins, a group of chemicals that play a role in pain and inflammation. Because these drugs can increase the risk of cardiovascular and GI issues, be sure to speak to your doctor before taking them either for short- or long-term use. Your doctor may opt instead to prescribe a topical anti-inflammatory like Voltaran Gel, which is minimally absorbed systemically and less likely to cause side effects.
2. Invest in proper footwear
“When you have arthritis, your shoes are either going to help you or hurt you,” says Jackie Sutera, DPM, a podiatric surgeon in New York City. Proper fit is a key factor in how foot-friendly shoes are. Besides having to accommodate an arthritic joint that may have stiffness, swelling, and contracture, shoes need to fit the hammertoes and bunions that often happen along with arthritis. Comfort brands like Vionic, Ecco, Clarks, and Mephisto are designed to be stylish and comfortable. They include arch support, heel cups, thick soles, cushioning, and shock absorption.
People with bad osteoarthritis in the feet may particularly benefit from shoes with rocker soles, which have a thicker-than-normal sole with a curved heel. A shoe with this type of sole (common in athletic footwear) reduces pressure under the big toe joint by 12 percent in people with OA, research shows. In a recent study the pain score in those who wore rocker sole shoes improved by 22 points.

3. Set a weight loss goal
When it comes to arthritis, what your scale says really matters. People with a higher body weight are diagnosed with arthritis at an earlier age and have more severe arthritis. It makes sense: “Feet are a weight-bearing joint, so obesity makes arthritis worse,” says Dr. Domingues. Even one extra pound on your frame can equal about five extra pounds of force on your feet. Losing 20 pounds can mean sparing your feet from an extra 100 pounds of force with every stride.
Excess body weight also increases inflammation, which fuels the painful symptoms of inflammatory types of arthritis like rheumatoid arthritis and psoriatic arthritis. It’s not easy to lose weight when you have stiff or sore joints, but even a five- to 10-percent reduction in body weight has been shown to dramatically diminish joint pain and improve exercise tolerance. Check out these weight loss tips that are especially helpful when you have arthritis.
4. Move more
It can be hard for even the healthiest people to maintain an exercise program, so for those with joint pain it can be especially difficult. But the benefits of exercise when you have arthritis are clear: Research shows regular moderate exercise helps maintain joint function while reducing pain and fatigue and relieving stiffness. And of course, it can be very helpful at burning calories, so you can shed weight. Make sure you don’t believe this outdated myth about exercise and arthritis.
Aim to stay as active as possible — any movement counts, including walking the dog, puttering around the garden, and standing while you talk on the phone — and find comfortable ways of being active. Instead of running outside, try walking on the treadmill, which provides more shock absorption. Or try other lower-impact exercises like swimming, rowing, biking, or using the elliptical machine. “You’ll still get cardiovascular benefits from them without pounding your feet,” says Dr. Sutera. Your goal is to work up to 150 minutes of aerobic exercise a week, split into shorter periods (even five- or 10-minute blocks of time) if that’s easier on your joints.

5. Employ ice or heat
“I’m a big believer in ice — it’s a great anti-inflammatory,” says William Spielfogel, DPM, chief of podiatry at Lenox Hill Hospital in New York City. “But I have patients who swear by heat.”
Each therapy works differently to provide pain relief: Cold therapy constricts the blood vessels in the surrounding muscles, which decreases blood flow to the joints to reduce swelling and inflammation. Heat therapy helps loosens the muscles to decrease spasms and reduce joint stiffness. Both also act on receptors in your skin to interrupt pain signals sent to the brain.
Depending on what type of pain you’re experiencing you might want to consider using both ice and heat. For instance, if you’re stiff in the mornings, a warm shower can ease symptoms, so you can move better. When your RA flares or you have inflammation from OA (maybe you spent an entire day on your feet), a cold pack or bag of frozen peas (wrap it in a paper towel before applying to skin) can help put pain and swelling on ice.
6. Investigate inserts
Custom-made orthotics can help soothe arthritic foot pain. “The beauty of orthotics is that there are lots of ways we can individualize their use,” says Dr. Sutera. They can be customized to change the mechanics of your foot — for instance, to limit the big-toe joint so it can’t move while you walk (and thus reduce discomfort). Or they can be made to be more accommodating to your feet, say, by adding supportive cushioning.
Because the severity of arthritis foot pain can vary between the left and right foot, the customization of your orthotics can be different on each side of the foot. Research on orthotics and foot pain is limited, but a 2016 study using shoe-stiffening inserts to treat MTP pain found clinically worthwhile improvement in foot pain and foot-related disability over a three-month period, with nearly 80 percent of participants saying they were effective.
7. Try alternative treatments
Though research has repeatedly shown that supplements like glucosamine and chondroitin don’t work well for most people, Dr. Domingues still sometimes recommends them for patients with osteoarthritis, who have fewer drug options than inflammatory types of arthritis. Glucosamine and chondroitin are natural components of the cartilage in joints that gets broken down in people with OA. “Anecdotally, we find people feel better on them,” he says. The brand he recommends is Osteo Bi-Flex, which contains glucosamine, chondroitin, and the herbal extract boswellia, among other ingredients.
Another promising treatment is turmeric, which some research shows may be helpful in treating osteoarthritis and inflammatory arthritis like RA. A spice that’s the main ingredient in curry, turmeric contains an antioxidant called curcumin that helps fight inflammation.
To further spice up your arthritis treatment, many physicians also recommend creams that contain capsaicin, a component of chili peppers. “It works very nicely topically, especially on feet,” says Dr. Sutera. In one study of 70 people with osteoarthritis and 31 with rheumatoid arthritis, 80 percent of people who applied capsaicin (versus a placebo) experienced some pain reduction. After four weeks, RA pain was reduced by 57 percent and OA pain was reduced by 33 percent.
8. Consult a physical therapist
“Physical therapy absolutely comes into play when trying to manage arthritis foot pain and there are all kinds of PT modalities that can be used to decrease inflammation, including massage, whirlpool, cold packs, ultrasound, and lasers,” Dr. Spielfogel says. Once the initial inflammation has been reduced, a physical therapist will develop a program of stretching and strengthening to restore flexibility and improve strength to increase balance and reduce stress on the foot joints.
Dr. Sutera finds that patients in the earlier stages of arthritis benefit the most from physical therapy, as they often still have flexibility and mostly need help restoring their balance.
9. Ask about steroid injections
Physicians often use steroids like cortisone to help with the acute inflammatory process and get patients stabilized. Cortisone acts as powerful anti-inflammatory; when injected into a joint it can help reduce swelling and inflammation and decrease discomfort. When cortisone is injected, its anti-inflammatory effects begin immediately, but the length of time it takes to experience pain relief can vary from days to weeks. There are a lot of misconceptions about cortisone injections because there are different types of cortisone. Generally, Dr. Sutera says, you can have three cortisone shots in as many months before taking a long break before getting another round.
10. Pamper your feet
If you have arthritis in your feet, chances are you also have it in your hands — and that can make it difficult to perform ped maintenance. But clipping your nails and smoothing calluses on a regular basis is important, says Dr. Sutera. “If you already have stiff joints, you don’t want to compound the problem by having long toenails, which can take up space in your shoe and create painful pressure.”
Consider treating yourself to a salon pedicure every four to six weeks. Just be sure to choose a salon that values cleanliness, for instance, by using disposable liners inside the foot tub and allowing you to bring your own nail files, pumice stones, and buffers. “Only metal tools can be cleaned, so it’s safer to bring your own,” says Dr. Sutera. If you have diabetes or circulation issues, check with your physician to make sure it’s okay to have a salon pedicure. Developing an infection can lead to serious complications in these cases.
11. Learn about your surgery options
When foot arthritis is severe and conservative treatment options fail, surgical intervention may be an option. One type is a fusion of the big toe joint, which fuses together the two bones that make up your joint. This limits the joint’s range of motion, helping to eliminate the source of pain. Another option is joint replacement surgery for the toe joints. Both are considered end-game measures, but for people who are healthy enough to withstand surgery, it can allow them to function much better.
Keep Reading
If you enjoyed reading this article, you’ll love what our video has to offer.
Subscribe to CreakyJoints
Receive our newsletter and stay informed about arthritis treatments, comorbidities, and more.





