
If you’ve had a nagging sore throat, your doctor may take a swab to check for strep. If you’re suffering from a high fever and bad cough, your doctor may order a chest X-ray to look for pneumonia. But not all diagnoses are that straightforward.
Case in point: Fibromyalgia, a condition that causes widespread chronic pain pain — as well as fatigue, sleep disturbances, and cognitive difficulties — is often challenging for a physician to pinpoint.
“Fibromyalgia can be difficult to diagnose because there’s no gold standard test like an X-ray or blood work,” says Lenore Brancato, MD, a board-certified rheumatologist at NYU Langone Ambulatory Care in New Hyde Park, New York. “It’s a diagnosis of exclusion, which means you first have to rule out other diseases that may be causing symptoms. It’s not a cookie-cutter condition.”
Fibromyalgia is also a diagnosis that’s been subject to change. Back in 1990, when the first diagnostic criteria were set by the American College of Rheumatology (ACR), a doctor had to find the following elements in order to say their patient had fibromyalgia: pain in at least 11 of 18 designated “tender points” throughout the body, plus a history of widespread pain lasting more than three months.
In 2010, however, those diagnostic criteria for fibromyalgia were updated to eliminate the tender point requirement and instead focus on findings that a patient has widespread pain, as well as sleep disruptions, fatigue, and cognitive difficulties.
Whereas the validity of fibromyalgia as a diagnosis was once questioned in the medical community — leading to a stigma it’s still overcoming — ongoing research has led to a number of possible explanations for physical causes of fibromyalgia (ranging from genetics to physical triggers) and mechanisms (involving the central nervous system).
What we know for sure is that fibromyalgia affects approximately 2 percent of adults in the United States, and your risk of developing the condition increases if you are middle-aged or older and have been diagnosed with lupus or rheumatoid arthritis, says the Centers for Disease Control and Prevention (CDC). You may also be at a higher risk if you are female (most fibromyalgia patient are women), have suffered a trauma or repetitive injury, or if you are obese.
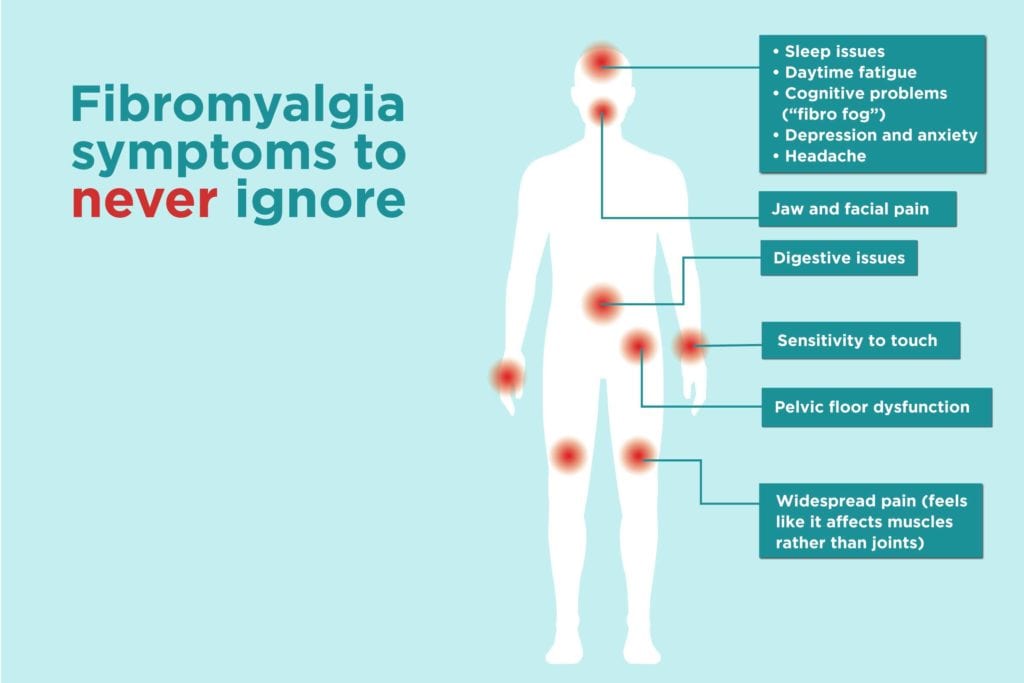
But statistics and risk factors can’t describe how fibromyalgia actually feels to the person living with it. What follows are the descriptions doctors hear patients use when they talk about both usual and less common symptoms of fibromyalgia.
Widespread pain
While every fibromyalgia patient is different, their descriptions of overwhelming, debilitating pain throughout the entire body are very common. “My patients report feeling sore and stiff with an achy pain that goes from the top of their head to their toenails,” says Christopher Morris, MD, a board-certified rheumatologist with Arthritis Associates in Kingsport, Tennessee, and a fellow of the American College of Rheumatology. “They tell me the pain is in the muscles and soft tissues rather than joints.” Dr. Brancato hears similar concerns, with some of her patients saying the pain is lacerating, “like being cut by knives.”
Sensitivity to touch
Fibromyalgia could also make you overly sensitive to touch and temperature. “If you’re a patient with fibromyalgia, and someone brushes up against you in a crowded room it can be very painful,” says Dr. Brancato. “I’ll hear that my female patients can’t tolerate a massage.” Even though the stimulus is taken away, like removing your hand from a hot stove, the pain can continue, she explains.
Sleep issues
If you have fibromyalgia, you may have trouble falling asleep or staying asleep. “My patients say they toss and turn, or their mind wanders,” Dr. Brancato says. “I’ll hear that my patients wake up throughout the night and end up feeling as tired as when they went to bed,” Dr. Morris adds.
Daytime fatigue
One of the most common issues for fibromyalgia patients is fatigue. “It’s exhausting for them,” says Dr. Brancato. “If you ask a patient how they feel in the morning, you’ll hear they felt awful, they never feel ready to go, they feel like they can’t get their head above water.”
Cognitive problems
“My patients describe having a ‘fibro fog,’” says Dr. Morris. “They have a hard time concentrating.” For her part, Dr. Brancato sees a lot of memory problems. “If you tell a fibromyalgia patient three things during an office visit, then ask them to recall them later during the same visit, they have difficulty,” she explains. “With fibromyalgia, short-term recall can be very poor.”
Depression and anxiety
For many patients, fibromyalgia may also bring feelings of sadness and other negative moods. Some researchers suspect a connection between fibromyalgia and certain types of chronic anxiety and depression.
Headaches
Though less common, headaches can occur among fibromyalgia symptoms. “Stress- and tension-type headaches tend to travel with fibromyalgia,” Dr. Brancato reports, adding that they can be triggered differently than in patients without fibromyalgia. “These headaches can be induced by regular sounds, background music, or even odors like perfumes.”
Digestive issues
Fibromyalgia can sometimes occur alongside digestive problems, such as bloating, constipation, abdominal pain, and irritable bowel syndrome (IBS), says the CDC.
Pelvic floor dysfunction
Some patients with fibromyalgia might also have an increased incidence of interstitial cystitis, says Dr. Brancato. This condition can cause chronic pain or pressure in the bladder and pelvis.
Jaw and facial pain
It’s possible for fibromyalgia to be linked to pain in the muscles of the jaw and face (temporomandibular joint disorder) or to myofascial (skeletal muscle) pain in one part of the body. Such occurrences could be considered forms of regional or localized or incomplete fibromyalgia.
Fibromyalgia and Arthritis: What’s the Link?
The relationship between fibromyalgia and different types of arthritis can be complicated. For one thing, there’s misdiagnosis: Depending on how your symptoms present, you could be told you have fibromyalgia when you actually have a kind of arthritis, or vice versa. Read about how ankylosing spondylitis and fibromyalgia can be mistaken for each other, for example.
At the same time, having a painful chronic disease like arthritis may in turn trigger the onset of fibromyalgia. Inflammatory diseases like arthritis can affect the way your central nervous system processes pain, creating a double-whammy of having both diseases at the same time.
If you suspect your combination of symptoms could be fibromyalgia, it’s a good idea to start with your primary care doctor. Because fibromyalgia is a diagnosis of exclusion, you’ll likely need a through physical exam, blood tests, and imaging tests to figure out what could be causing your symptoms. Ask about seeing a rheumatologist. These are doctors who specialize in diagnosing and treating musculoskeletal and related diseases.
Keep Reading
- A New Blood Test for Fibromyalgia Might Make Diagnosing Patients a Whole Lot Easier
- 18 Fibromyalgia Survival Tips from Fellow Patients
- Marijuana for Fibromyalgia Pain: Is It Worth a Try?
Subscribe to CreakyJoints
Get the latest arthritis news in your inbox. Sign up for CreakyJoints and hear about the latest research updates and medical news that could affect you.