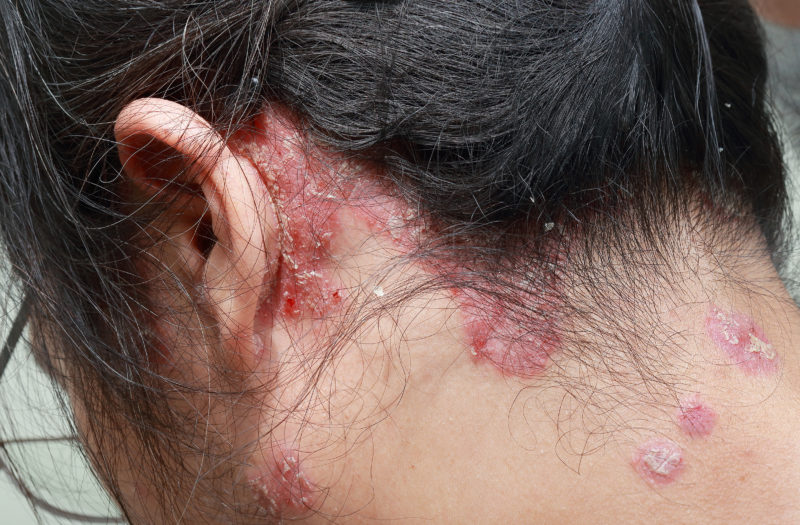
If you’re one of the roughly 2 percent of Americans who have psoriasis, a chronic condition that typically causes raised, red patches of skin topped with silvery scales, there’s a good chance that it has impacted your scalp. This also holds true for the more than 40 percent of people with psoriasis who also have psoriatic arthritis (PsA), a form of arthritis that can appear in combination with psoriasis.
Psoriasis causes skin cells to divide about 10 times faster than normal. The excess cells pile up on the surface of the skin, causing scaly patches of itchy, dry skin. Known as plaques, these lesions often itch, burn, and sting.
How Psoriasis and Psoriatic Arthritis Affect the Scalp
For many patients, the scalp is the only part of the body where psoriasis occurs — or it’s the first location where the autoimmune disease develops.
Research shows that at least a quarter of people with plaque psoriasis, the most common type of psoriasis, initially present with lesions on the scalp.
“It’s very common for psoriasis to affect the scalp — statistics show a range of 40 percent to 80 percent of people with psoriasis have scalp involvement,” says Mount Kisco, New York, dermatologist David Bank, MD, who is also an assistant clinical professor of dermatology at Columbia Presbyterian Medical Center in New York City. “It may occur in isolation or with psoriasis in other areas.”
Scalp psoriasis can run the gamut from mild (with thin dandruff-like flakes that are hardly noticeable) to severe (in which plaques can be so thick and inflamed that they’re visible through your hair).
Sometimes, in addition to the scalp, plaques also cover nearby areas such as the forehead, back of the neck, and the skin around the ears.
The Impact of Scalp Psoriasis and Hair Loss
It’s not really known why the scalp is so susceptible to psoriasis. One possible reason it’s such a prime area is that the high follicular density of the scalp (meaning: there are a lot of hair follicles there) reduces natural light exposure. Ultraviolet rays from light exposure can help clear or prevent psoriasis.
Although scalp psoriasis alone involves a small percentage of the body, it can have a profoundly negative affect on a person’s quality of life and self-esteem. But when it leads to hair loss —psoriatic alopecia in doctor-speak — it can be particularly distressing.
“The decrease in hair density is typically mild and difficult for the doctor to see, but of course, we take it very seriously,” says Vinicius Domingues, MD, a rheumatologist in Daytona Beach, Florida, and medical advisor for CreakyJoints.
Rest assured, once scalp psoriasis is under control, most people with hair loss experience complete regrowth of their hair.
The key is to seek medical help promptly, since scarring that results from psoriasis — common in longstanding scalp psoriasis — can cause permanent hair loss.
The Connection Between Hair Loss and Psoriasis and Psoriatic Arthritis
There are a few causes of psoriatic alopecia, including the disease itself.
Inflammation
“Psoriasis is an inflammatory condition and when the scalp is inflamed, the hair follicles [where hair is produced] can be affected,” says Mona Gohara, MD, associate clinical professor of dermatology at Yale School of Medicine in New Haven, Connecticut.
Damage from Scratching
Trauma to the scalp that often results from scratching or picking at the scaly spots can also trigger hair loss. “Scalp psoriasis can be particularly itchy. Scratching it to remove the scale can aggravate the problem and lead to more hair loss, a response known as the Koebner phenomenon,” says Dr. Gohara.
Increased inflammation can, in turn, increase itching, which creates an ever-worsening cycle that can ultimately (though, thankfully, rarely) lead to scarring. Hence the reason mane management requires early intervention. “Once the follicle is scarred, it’s not going to regrow hair,” says Dr. Gohara.
Medication Side Effects
Some medications used to treat psoriasis and psoriatic arthritis are also associated with hair loss, which tends to affect the areas covered in plaques. Hair loss is most common with methotrexate, a type of DMARD (disease-modifying antirheumatic drug) that works to quiet the immune system.
“It’s technically a chemotherapy medication and most of them affect the turnover of cells, including those responsible for hair growth,” Dr. Bank explains. While hair loss is not a very common side effect of methotrexate, it can cause 5 to 10 percent of people to experience hair loss.
Stress
Ironically, because stress is a trigger for psoriasis and psoriatic arthritis, the anguish over losing your hair can exacerbate plaques and potentially make hair loss even worse. “People don’t often talk about the stress associated with psoriasis, but having that in your hair and not being able to style your hair, or having to scratch or to have the flakes on your clothes, it’s embarrassing,” says Dr. Gohara. “All of that can create stress.”
Treatments to Clear Scalp Psoriasis and Stop Hair Loss
The good news is that there are many effective ways to treat scalp psoriasis. Once your skin clears, your hair will usually grow back.
The bad news is that scalp psoriasis can sometimes be difficult to treat. Hair makes the scalp inaccessible for topical therapies, which are thick and gooey and hard to get in and out of your hair.
“The practicality of applying a cream, ointment, or foam into the scalp makes it difficult for topical treatment of psoriasis of the scalp,” says Dr. Gohara. “If you don’t wash your hair every day, who the heck wants to slather creams and ointments on their scalp?”
This is especially problematic for Black and brown-skinned people, she says, who tend to wash their hair more infrequently.
Treatment depends on the severity of the condition.
Topical steroids
For mild-to-moderate cases of scalp psoriasis, your doctor will likely recommend topical treatments. Corticosteroids, which work to normalize cell production, are the mainstay of topical treatments, though they’re often used in conjunction with phototherapy and systemic and targeted drugs.
Steroids are available in prescription creams, ointments, foams, and are prescribed for twice-daily use for two weeks.
Usually, doctors recommend that you apply the steroid to your scalp at night and then wash your hair in the morning. “For people who shower at night, it becomes more challenging because they don’t want to use the treatment during the day,” says Dr. Domingues, who prescribes a steroid shampoo in those cases. “Allowing it to sit on your scalp for about 10 minutes helps make it more effective,” he says.
Topical therapy may exacerbate hair loss by friction and breakage of the hair, so it’s important to gently apply medication only to roots.
Steroid injections
If the topicals don’t clear the plaque lesions and control symptoms, or the plaques are very thick and scaly, steroid injections directly into the scalp can be administered. Though these can be painful, they can address the psoriasis and be more compatible with people’s hairstyles and hair-care practices.
Medicated shampoo
Steroids are often used in conjunction with over-the-counter shampoos formulated with coal tar and salicylic acid, ingredients that act to slow skin cell growth and soften and remove scales so prescription topicals can penetrate better.
Shampoos to look for include:
- Neutrogena T/Sal shampoo (contains salicylic acid)
- Dermarest Psoriasis Medication Shampoo Plus Condition (contains salicylic acid)
- MG217 3% Coal Tar Formula Shampoo
- Psoriatrax 5% Coal Tar Psoriasis Shampoo
Medicated shampoos work best if left on the scalp for five to 10 minutes.
Systemic treatment
For psoriasis and psoriatic arthritis, systemic therapy means taking a medication — such as an oral pill, an injection, or an infusion — that helps stop the immune system overactivity that is causing plaques to develop.
Systemic treatment for psoriasis or psoriatic arthritis that is affecting the scalp generally falls into three main categories:
- Conventional disease-modifying antirheumatic drugs (DMARDs), which are usually taken orally and include medication such as methotrexate
- Targeted disease-modifying antirheumatic drugs (DMARDs), which are oral pills that are more targeted than conventional DMARDs
- Biologic disease-modifying antirheumatic drugs (DMARDs), which are administered as injections or infusions and are more targeted than conventional DMARDs
It isn’t usually considered unless scalp psoriasis is moderate to severe, but Dr. Gohara reports that even in mild-to-moderate cases of scalp psoriasis, many patients request to be put on biologics, a type of drug that targets specific parts of the immune system that are overactive.
“Scalp psoriasis is like this bugaboo where people go from zero to 100,” says Dr. Gohara. “Patients are like, ‘I’m not going to do the creams, I’m going to do the biologics.’ Scalp psoriasis really bothers people, especially if it’s bad. It can be inflamed and get infected easily.”
It often makes people very self-conscious. “If you have it on your elbow, you can cover it,” says Dr. Gohara. “You can’t cover psoriasis on your scalp.”
Targeted therapies that are FDA-approved to treat both psoriasis and PsA fall into several categories based on the specific immune system proteins they target.
Biologics (injections and infusions)
Approved biologic disease-modifying antirheumatic drugs (DMARDs) for psoriasis and psoriatic arthritis include:
Tumor necrosis factor (TNF) inhibitors
- Adalimumab (Humira)
- Certolizumab pegol (Cimzia)
- Etanercept (Enbrel)
- Golimumab (Simponi, Simponi Aria)
- Infliximab (Remicade)
Interleukin inhibitors (IL-23 and IL-17)
- Guselkumab (Tremfya)
- Ixekizumab (Taltz)
- Secukinumab (Cosentyx)
- Ustekinumab (Stelara)
T-cell inhibitors
- Abatacept (Orencia)
Targeted synthetic DMARDs (oral pills)
Approved targeted synthetic disease-modifying antirheumatic drugs (DMARDs) for both psoriasis and psoriatic arthritis include:
Janus kinase (JAK) inhibitors
- Tofacitinib (Xeljanz)
PDE4 inhibitors
- Apremilast (Otezla)
As effective as they are, targeted therapies don’t completely erase the need for topical treatment. “They might clear your psoriasis, but most derms will have you on a topical as well — it’s like the cherry on top to help keep your scalp clear,” says Dr. Gohara. The need for topicals should be lessened, though, when you’re on a systemic therapy.
It’s important to be aware that people lose hair for many reasons, so if treatment isn’t stopping your hair loss, be sure to tell your health care provider. Your hair loss could be caused by something other than scalp psoriasis.
For instance, people with psoriasis are at greater risk of developing alopecia areata, an autoimmune disease that develops when the body attacks its own hair follicles, which can cause hair loss. Your health care provider can help determine the cause of your hair loss.
Tips for a Healthy Scalp and Hair with Psoriasis and Psoriatic Arthritis
Psoriasis and psoriatic arthritis are chronic conditions that can flare up. These tips for treating your tresses (and your scalp) with TLC can help prevent or manage a flare and a subsequent bout of hair loss:
Brush and comb hair gently
“Psoriasis scale can adhere to the hair, which gets pulled out when the scale is removed,” says Dr. Bank. Instead of forcefully removing the scale by picking at it, aim to first loosen it by gently brushing or combing and then remove it by washing with a salicylic acid or coal tar shampoo. Be sure to keep nails short to minimize hair breakage and gently blot and squeeze — don’t rub — post-shampoo with a soft T-shirt or microfiber towel to remove excess water.
Scratching, scraping, or irritating your scalp can trigger a psoriasis flare.
Shampoo regularly
“Psoriasis responds well to frequent hair washing,” says Dr. Bank. “People often decrease hair washing because they erroneously think their scalp is dry and that the additional shampooing is worsening the condition.”
Dryness is due to the buildup of skin cells; shampooing regularly with a medicated shampoo (twice a week for maintenance) breaks down or softens the crusty scales so they’re easier to remove without damaging the hair or further irritating the scalp. It helps make topical medications more effective as well.
Condition regularly
Dry hair is more likely to break, which can lead to hair loss. If medicated shampoo is overly drying, alternate it with a gentler, non-medicated shampoo.
Be cautious about coloring your hair
Don’t dye your hair unless your psoriasis is under control, advises Dr. Domingues. “Putting chemicals on an already inflamed area can worsen your condition.”
Minimize the use of heat
Allow your hair to air dry or use a blow dryer on the lowest setting. Don’t let curling irons, flat irons, or other thermal instruments touch your scalp. The heat can irritate or burn your scalp, which can trigger a flare.
Avoid tight hairstyles
Pulling too tightly on the hair can irritate the scalp and cause a flare. Over time, the continuous tension on the hair follicles caused by the constant pulling of hair can lead to hair loss.
Track Your Psoriatic Arthritis Symptoms with ArthritisPower
Join CreakyJoints’ patient-centered research registry and track symptoms like fatigue and pain. Learn more and sign up here.
Want to learn more?
Listen to this episode of Getting Clear on Psoriasis, from the GHLF Podcast Network.
If you enjoyed reading this article, you’ll love what our video has to offer.
Blakely K, et al. Management of scalp psoriasis: current perspectives. Psoriasis Targets and Therapy. March 2016. doi: https://doi.org/10.2147/PTT.S85330.
Interview with David Bank, MD, assistant clinical professor of dermatology at Columbia Presbyterian Medical Center in New York City
Interview with Mona Gohara, MD, associate clinical professor of dermatology at Yale School of Medicine in New Haven, Connecticut
Interview with Vinicius Domingues, MD, a rheumatologist in Daytona Beach, Florida, and medical advisor for CreakyJoints
Managing Scalp Psoriasis. The Dermatologist. August 2012. https://www.the-dermatologist.com/content/managing-scalp-psoriasis.
Scalp Psoriasis: 10 Ways to Reduce Hair Loss. American Academy of Dermatology Association. https://www.aad.org/diseases/psoriasis/scalp-psoriasis-10-ways-reduce-hair-loss.
What you need to know about alopecia areata. National Alopecia Areata Foundation. https://www.naaf.org/alopecia-areata.