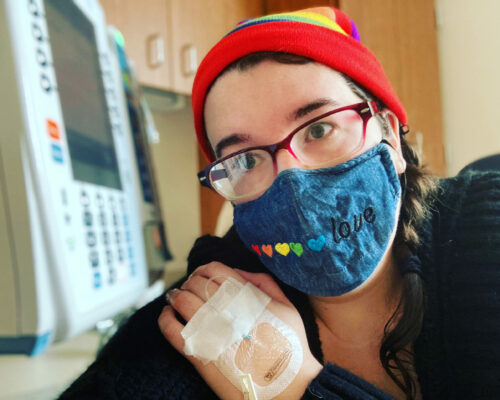
It was Christmas Eve, and I was settling in to watch a movie with my teenager — with new pajamas on and a mug of hot cocoa waiting to be sipped — when I got an unsettling email.
“Unfortunately,” it read, “we’ve just been informed that one of the performers tested positive for COVID this morning.” The night before I had performed in a burlesque show with about seven other people, and it seems one of those people had COVID, despite being vaccinated and boosted.
I quickly replayed the night in my head. Aside from a short period of time when I was doing my makeup, and then the 10 minutes or so total that I was onstage, I had stayed masked. All of the performers, as well as all the audience members, had been required to show vaccination cards upon entering the building. I’d maintained as much distance from folks as possible in the green room backstage. Surely, I thought to myself, with all those precautions in place there was no way I could have gotten COVID.
A Calculated Risk Is Still a Risk
As an immunocompromised person with chronic health issues, I had started isolating from the very beginning of the pandemic, before many of my friends were even aware that the coronavirus could be an issue. Like many other chronically ill people, for months I didn’t leave the house at all, canceling all appointments and getting everything delivered. However, once the vaccine was available, and as it became more apparent that the pandemic was going to be very long-lasting, I began taking small calculated risks — dinner with a close friend at an outdoor restaurant, a quick trip to the craft store, and performing in shows.
I’m a burlesque performer. When I’m onstage, I feel free in a way that nothing else quite compares to. In fact, when I was questioned about my performing in my disability hearing, despite the fact that performing hurts my body and will often put me in bed for a few days after, I told the judge that the reason I keep doing it is because it is one of the few things that continues to bring me unadulterated joy.
So, when some producers began offering outdoor shows, or shows where all performers and patrons had to be vaccinated, I took a calculated risk — and decided to perform one or times a month.
Unfortunately, even a calculated risk is still a risk. When I woke up December 26 with a sore throat and a pounding headache I knew, despite all my precautions, that I had COVID.
I Was Overwhelmed
I sequestered myself into my bedroom so as to not further expose my teenager. I called my family I’d seen on Christmas Eve to warn them and texted my friends: “I think I might have COVID,” I wrote. “I am hoping it is just a cold though.” I called the nurse at my local COVID clinic who told me that I could test five to seven days after exposure. A friend dropped off some rapid tests and yelled “I love you!” through the door.
That day my test came back negative, but I continued to feel worse over the upcoming days, so on December 28 — five days after exposure — I tested again. This time it came back positive. I immediately called back the nurse at the COVID clinic. It was then that I learned two important pieces of information.
First, because of being on immunosuppressant medication, I was eligible for an antibody infusion, which we got scheduled for just a few days later.
Second, those of us who are immunocompromised may have a different isolation period. Instead of having to quarantine for five days like others needed to do, I was required to quarantine for 20. (Note: This doesn’t necessarily apply to everyone who is immunocompromised, so be sure to talk to your doctor to find out what’s right for you.)
I was overwhelmed. Not only did I not feel well, but I also realized that meant for 20 days I would need to rely on others to help me with food, medications, and anything else I needed. It meant that for 20 days I’d need to stay mainly in my bedroom in my small apartment in order to keep my teenager safer.
It meant for 20 days I was going to be very much alone.
For me, one of the hardest parts about chronic illness is the isolation that comes along with it, while, conversely, one of the most gratifying things is the community I’ve built with other sick and disabled folks and very supportive non-disabled friends. While I knew that 20 days without physical interaction with anyone else was going to be hard, I also knew I was lucky enough to have a support network who would help me get through.
Friends dropped off cat litter and groceries, picked up medications at the pharmacy, sent gift cards for meal delivery, and messaged me with cute animal videos to cheer me up. Despite having to be alone, I was surrounded by love and care, and was so grateful for that.
I Had More Pain and Stiffness
I spent many of those initial days sleeping, as COVID made me weary in ways even my chronic fatigue didn’t. Aside from getting up to use the bathroom, get food, and have my one outing to get the antibody infusion, I spent my days in bed, either doing embroidery, watching a show — or more often than not, sleeping.
I also started to get really achy, but not just from COVID. To control the symptoms of ankylosing spondylitis I’m on a biologic infusion called Remicade (infliximab), which I receive every four weeks. This is the medication that makes me immunosuppressed.
You can’t receive the infusion if you’re sick, so my infusion that was scheduled at the end of December had to be canceled. I then learned that you had to be completely free of COVID respiratory symptoms for at least 20 days before receiving the infusion again. This meant I couldn’t have my infusion until the second week of February.
As more and more days passed between my infusions, I became more stiff and my pain increased. My doctor increased my anti-inflammatory medications, but even still, my mobility and comfort were greatly impacted. I began needing to use my mobility aids more often, as well as things like compression gloves and socks to help with joint pain. Even now, after having one of my infusions, I have not returned to my pre-COVID baseline.
My doctor says it may be a few more months and after a few more infusions before I feel okay again.
I Worried About Long-Term Ramifications
Despite feeling pretty miserable from the COVID symptoms — with headaches, sore throat, and chest congestion — I never got to the point that I was scared or worried about hospitalization. Even when my coughing got bad, I used my inhalers and nebulizer and things calmed down pretty quickly.
But as the fatigue and extreme exhaustion drew out, the more concerned I started to get about long-term ramifications of having COVID.
I quickly learned I wasn’t the only one. Charlie Flewelling, who lives with Ehlers-Danlos syndrome and bipolar disorder, told me they felt similarly when they got sick with COVID. “On being diagnosed I wasn’t too scared having had years to prepare, and [because I was] vaxxed and boosted. As symptoms tore through me, I felt a little worse and more scared of long-term effects,” they said.
Paige DeAlmeida, a childhood cancer survivor with long-term effects, shared with me a similar experience. She knew if she got COVID she’d be impacted long-term, which she told me, “is frustrating and annoying, but my reality.”
Living with chronic illness often means juggling new symptoms or conditions. It is something that many of us are used to. But that doesn’t make it any easier, nor does it make the fear of uncertainty and ‘what-ifs’ any less powerful. I am now nearly two months out from the onset of my initial COVID symptoms, and most everything has dissipated, except for a heart rate that elevates far too quickly and fatigue that knocks me out for a few hours daily.
As with all new symptoms I develop, I’m going through a grieving process with this, working my way to accepting this as a potential new reality. As Flewelling said, it is a process “trying to love and accept the impaired body/mind while fearing the acquisition of more impairment.”
This is a journey that will take time.
Get Free Coronavirus Support for Chronic Illness Patients
Join the Global Healthy Living Foundation’s free COVID-19 Support Program for chronic illness patients and their families. We will be providing updated information, community support, and other resources tailored specifically to your health and safety. Join now.