Learn more about our FREE COVID-19 Patient Support Program for chronic illness patients and their loved ones.
COVID-19 has been associated with a wide range of symptoms, including fever, fatigue, cough, shortness of breath, diarrhea, and even a new loss of taste or smell. More recently, reports from across the world indicate that the disease also has skin-related symptoms — including rashes and purple spots on the feet, toes, and (less commonly) the hands, which are being dubbed “COVID toes.”
While it took several months from the original outbreak of the disease for skin manifestation to be reported, it’s not that surprising that signs of COVID-19 are showing up in the skin. “The skin is often a clue to what’s going on inside the body,” says Lindy P. Fox, MD, professor of clinical dermatology at the University of California, San Francisco, and a leading expert on the dermatological changes associated with the coronavirus.
That COVID-19 affects the skin makes sense physiologically. It’s not out of the ordinary for viruses to affect the skin because the chemicals released by the immune system to destroy a virus like the coronavirus can also cause inflammation that results in a rash. “Since these rashes are so common in response to other infections, it’s not surprising that they’ve been reported with COVID too,” says Dr. Fox. In fact, an early report of COVID-19 rashes in Italy, the researcher said the rashes he was seeing were like the skin manifestations he’d observed with other common viral infections.
Toe lesions, on the other hand, are surprising, and as a result, they’re grabbing the spotlight. Which is good, says Dr. Fox. “We’re trying to get it on the radar so that people understand that, if this [symptom] comes their way, they should think of COVID.”
When you have autoimmune or inflammatory arthritis, you may already be prone to looking out for new or unusual skin symptoms. The inflammatory condition psoriasis is very common in certain types of arthritis (namely psoriatic arthritis and spondylitis). These conditions can also cause dactylitis, or swelling of the fingers or toes. Rashes are common in lupus and rheumatoid arthritis. RA is also known for causing nodules below the skin; gout is known for causing tophi, or lumps of uric acid crystals. Many common medications, including methotrexate and hydroxychloroquine, can cause photosensitivity, making rashes even more common as people spend more time outdoors during summer.
That makes it all the more important to understand potential skin symptoms associated with coronavirus and talk to your health care provider about anything that seems new or worrisome. As new cases of COVID-19 continue to occur and as rashes gain more recognition among both providers and patients, we are providing key information about skin manifestations of COVID and what to do if you notice a new rash or skin lesion.
1. There are two types of skin manifestations of COVID-19
Nonspecific Rashes
The first type are nonspecific rashes. Most commonly, these include:
- Hives (officially called urticaria), which look like red welts
- Morbilliform rash, which looks like small pink bumps or flat spots and usually occurs on the trunk, hands, or feet
Both of these rashes can happen in response to many potential causes, including other infections and medications. They are not characteristic enough to identify the specific virus that’s causing it (hence the term nonspecific). Be assured that having a rash of this type does not mean you have COVID. “COVID is just on the list — the long list — of things that can cause rashes like this,” says Dr. Fox.
COVID Toes
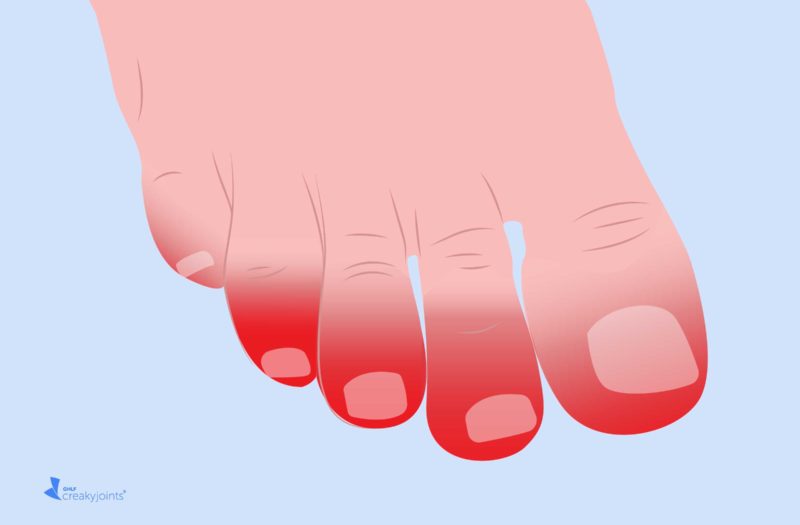
The second skin symptom, “COVID toes,” is considered a specific rash — along the same lines as the well-known rashes caused by measles and the chickenpox virus. “It is remarkable, unusual, and characteristic,” says Dr. Fox of the red, sore, and sometimes itchy swellings on toes.
COVID toes look like chilblains (officially called pernio), which is an inflammatory condition that normally occurs on the hands and feet of people who’ve spent a long time outdoors in the cold. “In a normal year, we would see only a handful of patients with pernio in cold months, or in people who travel from warm to cold climates,” says Dr. Fox. “But we’re seeing a really huge number of cases — far beyond what we’d normally see — in the wrong time of year and in places like Florida and Texas, all while we’re in the middle of a COVID crisis.”
As a result, she says the current thinking is that chilblains or chilblains-like spots on the toes are a sign of COVID until proven otherwise. “It’s like loss of smell — if you haven’t got another good cause of loss of smell, consider COVID [as a possibility],” she says. “This should be the same thing.”
2. Not all COVID-19 patients have skin symptoms
When it comes to skin manifestations of COVID-19, “there are currently more questions than answers,” notes researchers in the Cleveland Clinic Journal of Medicine. For one, it is still unclear what percentage of patients develop skin involvement. Skin rashes currently are not yet a criteria for testing in most states, so people would not likely have gotten tested for that reason alone. Plus, testing was not readily available early on in the pandemic, and many people with mild symptoms of the disease don’t even get tested.
That early study of COVID-19 rashes, which was a published in late March, found that slightly more than 20 percent of 88 patients with COVID-19 had skin symptoms. Forty-four percent (eight patients) had skin rashes at the onset of symptoms while the rest developed a rash after being hospitalized. In another study, Chinese researchers reported that only 1.8 percent of patients (two of 1,099 people) developed skin abnormalities.
While these studies help raise awareness about skin involvement with COVID-19, their findings are limited. For instance, since the samples weren’t population samples, “you can’t say that 20 percent of people with COVID get rashes,” says Dr. Fox. To know how commonly rashes occur in COVID-19, “we’d have to know every single person with COVID and then see how many of them had a rash.” Since testing has been so limited, it is likely that number will never be known.
The American Academy of Dermatology has created a COVID-19 registry, where doctors can enter information about suspected COVID patients with skin involvement. Doctors who have a suspected COVID patient with a skin finding, whether or not the infection is confirmed with testing, are encouraged to enter information about that patient into the registry. According to Dr. Fox, who is a member of the task force, “this can help figure out evidence-based answers to many of the questions doctors have about the many skin manifestations of COVID.”
3. People don’t exhibit rashes in the same way
Nonspecific rashes (red, blotchy areas) tend to occur most commonly when someone has COVID-19 and they’re pretty sick with it, says Dr. Fox. This likely means you would have other symptoms, such cough or fever, besides the rash.
Conversely, the trend with COVID toes is that it most commonly occurs in the late stage of the disease in children or young adults who are otherwise healthy. The symptom develops as a secondary inflammatory response past the time that most people are actively infectious.
“Rarely, patients who develop pernio-like changes will do so before they get COVID symptoms or at the same time as more typical symptoms,” Dr. Fox told MDedge in an interview. “But around half of them never had a known COVID infection or known contact, or were even symptomatic,” says Dr. Fox. All of a sudden, they show up weeks later with spots on their toes and, when tested, they’re no longer shedding the virus (which means they are no longer contagious). While this isn’t true for everyone, it is a trend, she says. As awareness of COVID toes increases, Dr. Fox thinks more patients might be seen at the more active stage of the disease.
If someone with COVID toes tests negative, they likely do not need to worry about infecting people within what Dr. Fox calls their “COVID pod” — family or roommates who have probably been with them the whole time. That is because any transmission likely would have already occurred. “They should still practice social distancing, wear a mask, practice good hand hygiene, and do all of the careful things that we should all be doing,” says Dr. Fox. “However, they can live in their homes and be reassured that most likely they are in the convalescent [recovery] stage.”
4. ‘COVID toes’ can be a clue to prognosis
“For the most part, COVID toes is not a poor prognostic sign and, if anything, it tends to happen in healthy young people who manage the virus very well and don’t get very sick with it,” says Dr. Fox.
There’s really no clue with nonspecific rashes. “I’d say [they usually affect] someone who is symptomatic, they feel pretty sick, and could have COVID, but [having a rash] doesn’t necessarily mean they’re going to do worse or end up in the hospital,” says Dr. Fox.
5. Most skin symptoms don’t need treatment
Depending on the type of skin manifestation and how symptomatic the patient is, doctors do treat rashes and COVID toes. “Rashes tend to self-resolve, but because they can be uncomfortable, we might recommend topical or oral treatments, such as steroids and aspirin,” says Dr. Fox.
Especially with COVID toes, “most patients want reassurance that their toes aren’t going to fall off and that nothing else terrible is going to happen to them, and that’s often enough,” she says.
6. Have skin symptoms checked out
If you think you might have a skin symptom of the coronavirus, the best thing you can do is contact your health care provider, says Dr. Fox.
“If you have a nonspecific rash, with a good history, you can tease out the risk of having had COVID or being exposed to it, and the likelihood that you may need testing.”
COVID toes, on the other hand, she says, are a clear indication that you should be tested.
Get Free Coronavirus Support for Chronic Illness Patients
Join the Global Healthy Living Foundation’s free COVID-19 Support Program for chronic illness patients and their families. We will be providing updated information, community support, and other resources tailored specifically to your health and safety. Join now.
Guan W, et al. Clinical Characteristics of Coronavirus Disease 2019 in China. The New England Journal of Medicine. February 28, 2020. doi: https://www.nejm.org/doi/10.1056/NEJMoa2002032.
Interview with Lindy P. Fox, MD, professor of clinical dermatology at the University of California, San Francisco
Lipper G, et al. Dermatologic changes with COVID-19: What we know and don’t know. MDedge. May 18, 2020. https://www.mdedge.com/dermatology/article/222359/coronavirus-updates/dermatologic-changes-covid-19-what-we-know-and-dont.
Recalcati S. Cutaneous manifestations in COVID‐19: a first perspective. Journal of the European Academy of Dermatology and Venereology. March 26, 2020. doi: https://doi.org/10.1111/jdv.16387.
Young S, et al. Skin manifestations of COVID-19. Cleveland Clinic Journal of Medicine. June 2020. doi: https://doi.org/10.3949/ccjm.87a.ccc031.