Key Takeaways
- More than one-third of people taking the uric acid-lowering medication allopurinol were “non-persistent” over time, meaning they stopped taking it or took it inconsistently.
- People who didn’t take allopurinol consistently had greater odds of being prescribed prednisone.
- Prednisone has a lot of potential side effects that can be problematic for people with gout, such as raising blood sugar (and there is a lot of overlap between gout and diabetes).
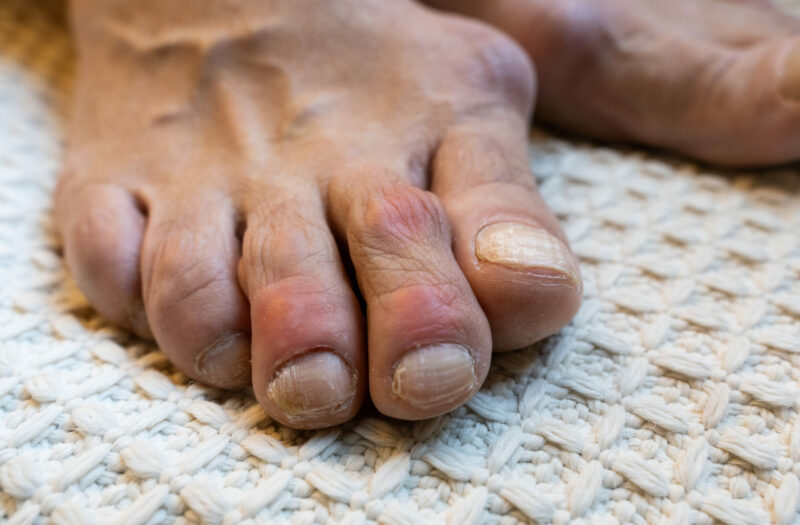
If you’re prone to gout attacks, your doctor may have prescribed allopurinol, a medication that helps prevent future flares by lowering levels of uric acid in your bloodstream. While it may seem obvious that stopping this drug or skipping doses puts you at risk for gout flare-ups, it turns out that it could also leave you vulnerable to another problem: You might end up needing corticosteroid drugs to manage gout flares.
In a new study, published in the journal Seminars in Arthritis and Rheumatism, Canadian researchers analyzed data on more than 22,000 new allopurinol users who had gout as well as diabetes. (The two conditions often overlap.)
They followed these individuals for three years and determined that more than a third were “non-persistent” with allopurinol, meaning that they used the medication inconsistently or completely stopped taking it during the study period.
Women were more likely than men to be in the non-persistent group, as were people with dementia and those who had had an outpatient visit for gout in the prior year.
According to the findings, “allopurinol interrupters and discontinuers had indicators of more severe gout over time compared to adherers, including greater odds of being prescribed prednisone.”
Prednisone is a commonly used steroid medication effective for reducing inflammation (including during gout flares), but carries a risk of numerous side effects. Possible prednisone side effects include stomach pain, mood changes, blood vision, and osteoporosis. It can also raise blood sugar, which is especially problematic for people who already have diabetes (including everyone in this study).
When viewed from a more positive angle, the flip side is also true: “Thus, among individuals with diabetes and gout, improving allopurinol adherence and persistence could potentially improve glycemic control through preventing prednisone use,” the authors speculated.
They concluded by noting that more studies are needed to understand why so many allopurinol users with gout and diabetes stop using this drug and develop strategies to promote better adherence.
Found This Study Interesting? Get Involved
If you are diagnosed with arthritis or another musculoskeletal condition, we encourage you to participate in future studies by joining CreakyJoints’ patient research registry, ArthritisPower. ArthritisPower is the first-ever patient-led, patient-centered research registry for joint, bone, and inflammatory skin conditions. Learn more and sign up here.
Jacobs S. Allopurinol Nonpersistence, Interruptions Among Patients With Diabetes and Gout Linked to Greater Prednisone Use. Rheumatology Advisor. December 6, 2021. https://www.rheumatologyadvisor.com/home/topics/gout/allopurinol-nonpersistence-interruptions-diabetes-and-gout-greater-prednisone-use.
Weisman A, et al. Allopurinol Adherence, Persistence and Patterns of Use in Individuals with Diabetes and Gout: A Retrospective, Population-Based Cohort Analysis. Seminars in Arthritis & Rheumatism. December 2021. doi: https://doi.org/10.1016/j.semarthrit.2021.09.003.