Check out Ghosting the Doctor in Ankylosing Spondylitis for more information on this topic.
Learning that you have ankylosing spondylitis (AS) is often no easy feat. People may experience back pain and other symptoms for years, seeing many kinds of health care providers and undergoing various tests along the way. It can be a frustrating process to feel unwell for so long without knowing what’s causing your pain. So why would people who find out they have AS — which usually requires treatment with medication and ongoing monitoring — then stop seeing the doctor?
This “ghosting” phenomenon is officially called “lost to follow-up” in medical terms. Just how common is it, and why does it happen? CreakyJoints conducted an online survey of members with axial spondyloarthritis, which includes ankylosing spondylitis and non-radiographic axial spondyloarthritis, to find out.
Conducted: August 1, 2021 to October 4, 2021
Number of respondents who completed the survey: 342
Demographics of respondents: 77 percent were female, 86 percent were white, with an average age of 52 and a median length of time of 8 years to get diagnosed
What We Asked
We wanted to understand a few general areas:
- Did people report that they stopped seeing a specialist (such as a rheumatologist) for a period of time after getting their AS/axSpA diagnosis?
- Why did people stop seeing the doctor after their diagnosis?
- How did this pause in care affect people’s symptoms and health?
- What caused people to start seeing the doctor again?
We developed an 18-question survey to delve into these topics.
What We Learned
1. The majority of respondents did not stop seeing their doctor, but almost one-quarter did
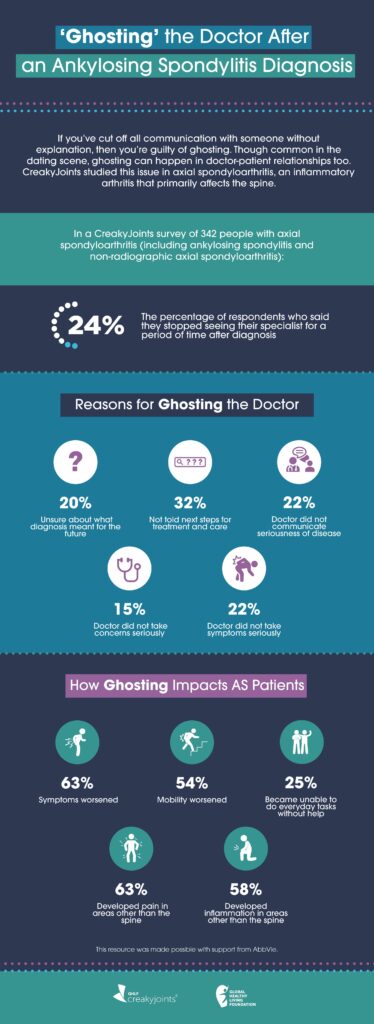
Out of 342 respondents, 81 (24 percent) said they stopped seeing their doctor for a period of time after getting their AS/axSpA diagnosis. Of those who kept seeing their doctor, the main reasons they gave for doing so was to get treatment so that their symptoms and health wouldn’t get worse.
2. There were many reasons people said they stopped seeing their doctor
Our survey results reveal that ghosting is not a simple issue — there are many reasons people stop seeing the doctor after an AS/axSpA diagnosis. Here are some of the most common responses. (People could select all that apply.)
- 32% said they were not told next steps for treatment and care
- 22% said their doctor did not communicate the seriousness of their disease
- 22% said their doctor did not take their symptoms seriously
- 20% said they were unsure what their diagnosis meant for the future
- 15% said their doctor did not take their concerns seriously
- 15% said they were scared about the diagnosis
- 13% said the doctor’s office was too far away
- 10% said they did not know what the disease was
Other issues included being unable to schedule appointments with the doctor or not being able to afford doctor appointments.
Respondents were able to write in responses to elaborate on other issues that affected their decision to stop seeing the doctor. Some themes included:
- Concerns about starting medication
- Concerns about being eligible for or affording medication
- Symptoms seemed manageable
- Satisfaction with current treatment
3. People who stopped seeing the doctor experienced worsening symptoms and quality of life
When we asked about the impact on people’s health and disease management of not seeing a doctor, only 7 percent said it had no impact. Here are some of the most common responses. (People could select all that apply.)
- 63% said their symptoms worsened
- 63% said they had pain in areas other than their spine
- 58% said they had inflammation in areas other than their spine
- 54% said their mobility worsened
- 25% said they became unable to do everyday tasks without help
- 20% said they did not begin treatment
4. Most people who stopped seeing the doctor did start again — and worsening symptoms was the main reason
Of those who said they stopped seeing the doctor, most respondents started doing so again. About one-quarter (27 percent) said they are still not seeing a doctor. Most people who started seeing a doctor again did so within six months to three years (37 percent). Another 25 percent said they did so within three years or more. About 11 percent of people said they returned to the doctor in less than six months.
When asked why they started seeing the doctor regularly again, here were the most common responses. (People could select all that apply.)
- 74% said their symptoms
- 26% said wanting to start taking treatment
- 24% said getting recommended to a different doctor
- 21% said learning more about their disease
- 12% said learning more about treatment
What This Tells Us
In a largely female and white population of CreakyJoints members who have axial spondyloarthritis, about one-quarter said they stopped seeing their specialist for an extended period of time after they were diagnosed. These results may not be generalizable to a broader group of axSpA patients.
Of this patient group, people reported a broad range of reasons for not seeing the doctor. Though far from comprehensive, these results indicate that addressing this problem may require tailoring approaches for individual patients and their providers. Strategies will need to address doctor-patient communication, health care access and affordability, and more.
Preventing loss of follow-up in ankylosing spondylitis is not nearly as simple as advising patients to not ghost the doctor — but it’s a good place to start the conversation.
The consequences can be serious. Stopping or delaying care because of “ghosting” can lead to worsening symptoms. Untreated AS can cause permanent joint damage and disability in some patients.
Patients and providers can recognize that: this phenomenon occurs, that many complex factors may play a role, and there is room for improved communication about what patients need to continue getting care for their condition.
This article is part of Ghosting the Doctor in Ankylosing Spondylitis and was made possible with support from AbbVie.
CreakyJoints Survey: Experiences Seeking Care for Ankylosing Spondylitis. October 4, 2021.