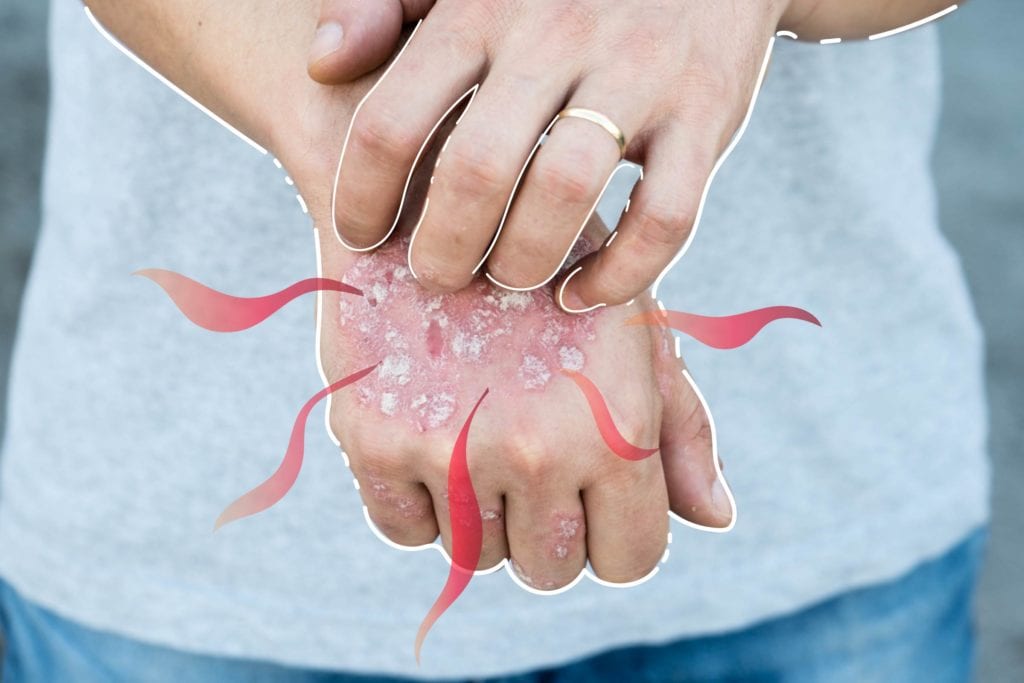

Psoriasis is well known for causing itchy, scaly patches called plaques, but it it’s more than just a skin condition. Psoriasis is considered an autoimmune issue, and it often goes hand-in-hand with other immune-related disorders like celiac disease and Crohn’s disease. People who have psoriasis also seem more likely to develop heart disease, cancer, and type 2 diabetes.
Although it’s extremely common to have psoriasis along with at least one other condition, this overlap of health issues (which doctors refer to as comorbidities) can make your psoriasis harder to treat. That’s the key finding from researchers who presented their work at the European Academy of Dermatology and Venereology congress in Paris earlier this month.
The researchers conducted a year-long observational study of 846 patients in the U.S. and Europe who were recently diagnosed with moderate or severe psoriasis. About 64 percent of the group had also been diagnosed with at least one other health problem by the time the study began.
While everyone in the study was using some sort of biologic agent — such as adalimumab (Humira) or etanercept (Enbrel) — to treat their psoriasis, those who weren’t simultaneously coping with another condition fared much better: Patients who didn’t have any additional health problems at the start of the study were significantly more likely to have their skin plaques clear up.
“Patients with no comorbidities at baseline reported almost double the clearance rate of those patients with three or more comorbidities at baseline,” Finn Ziegler, of LEO Pharma (who funded the study), told MedPage Today. In fact, 31 percent of them had achieved complete clearance of their plaques (PASI 100) within six months.
What Co-Occurring Diseases Are Most Common with Psoriasis?
The most common co-existing conditions among study participants were high blood pressure, psoriatic arthritis, high cholesterol and triglycerides (hyperlipidimia), diabetes, and depression.
Treating several health conditions at the same time is complicated for a number of reasons. In some cases, the ailments are directly related: For example, people who have severe psoriasis are more likely than those who have a mild case to develop psoriatic arthritis.
Even when there doesn’t seem to be a direct connection, having to juggle comorbid illnesses can take a toll. It’s harder to remember to take several medications and keep up with appointments with multiple specialists. People who have a mental health comorbid condition, like depression, also often have trouble taking good care of themselves in general.
If you’re having a hard time managing your psoriasis, talk to your doctor. You may need to try a different medication, though there are also a number of lifestyle changes (including managing stress, using a heavy ointment after showering, and bathing with Epsom salt or oatmeal) may make a difference along with your medical treatment.
Keep Reading
- Psoriatic Arthritis Can Cause Different Kinds of Bone Damage (and Surprisingly, Psoriasis Might Too)
- This Young Fitness Instructor Ignored Her Psoriasis and Psoriatic Arthritis for Far Too Long
- How Pregnancy Affects Your Psoriatic Arthritis